CLEARWATER, Fla. — A family is wanting answers after they say a local hospital used the court system to hold their brother in the hospital against his will for a year, racking up $1.2 million in medical bills before he died with toxic levels of drugs in his system.
In April 2021, Navy veteran Jimmy Johnston’s ashes returned to his hometown in Indiana for a final send-off.
A priest at the Catholic Church Johnston attended as a child spoke about the love he always gave to his family. An honor guard played taps and handed a carefully folded flag to his four siblings.

“Jimmy got the gene”
Jimmy’s hardest battle wasn’t waged against a foreign enemy, but in his head, against schizophrenia, a devastating chronic brain disorder that plagued his family.
“Each generation had someone. So, unfortunately, Jimmy got the gene,” said his sister Kathleen Johnston.
“It could have happened to any of us, you know. There, but for the grace of God, goes I,” Jimmy’s sister Patty Johnston said.
After he was honorably discharged from the Navy, Jimmy worked for a defense contractor and was injured on the job, leaving him physically disabled.
He moved from Indiana to Clearwater 20 years ago.
“Jimmy wanted to be on the water and he wanted to be warm. So he came down here. He had some friends down here,” Kathleen Johnston said.
His mental illness grew progressively worse.
In 2009, he began receiving help from the Florida Assertive Community Treatment (FACT) program, which provided care in a community-based, group home setting.
“They would make sure he got his meds every day and food and housing,” Kathleen said.
In January 2020, Jimmy’s sisters learned he had other health issues, leading him to seek care at Morton Plant Hospital.
“He had severe esophageal bleeds that would require blood transfusions,” Kathleen said.
At the hospital, Jimmy filled out forms designating his sister Kathleen to be his health care surrogate, a person who can make decisions for an individual about their health care if they are unable to.
“This is the hospital’s paperwork,” Kathleen said, showing the document.
“They insisted that we sign it,” Patty said.

Three months later, when Jimmy was admitted to Morton Plant Hospital again for a mental health episode, the hospital went to court to have him involuntarily committed for six months under Florida’s Baker Act.
The petition filed by the hospital with the court said, “The patient requires a highly structured setting for safety and cannot be maintained safely outside of a hospital setting."
Kathleen disagreed with that assessment.
“He didn’t bother anyone. He wasn’t suicidal. He was not violent,” she said.
“The hospital is never considered the first and best option”
Dr. Craig Beach never treated Johnston but has worked as a forensic psychiatrist, medical school professor and hospital administrator. He specializes in treating severe mental illness.
“The hospital is never considered the first and best option typically,” Beach said. “It’s really about considering what’s the least restrictive option where the person can be cared for and where they can be safe and where they can function.”
“He had loving brothers and sisters and the hospital knew that,” said attorney Vito Roppo, who represents Kathleen Johnston.
Roppo says the hospital didn’t make the judge aware of Jimmy’s health care surrogate document when requesting to have him committed.
“The hospital did not disclose that they had those documents that they themselves prepared and asked for,” Roppo said.
Instead of Kathleen making decisions, the court appointed a professional guardian.
His sisters say he had very little interaction with their brother and the court docket does not show any actions that guardians took on Jimmy’s behalf.
“For eight months, Jimmy’s under this guardianship. It’s a horrible system here in Florida, he’s under this guardianship and we cannot get any medical information,” Kathleen said.
In October 2020, the hospital requested a six-month extension of his commitment, saying in the petition, “Treatment cannot take place in a less restrictive environment because, despite medication adjustments, the patient continues to act psychotic."
“My brother… I don’t want to sugarcoat it… He definitely was very mentally ill. But he wasn’t gone. He didn’t have dementia. He could carry on a conversation with us,” Kathleen said.
The daily charge for room and board: $1,992
Invoices show Morton Plant Hospital billed $1,992 a day for Jimmy’s room and board in the psych unit and gave him daily cocktails of antipsychotic drugs, including Benztropine, Norclozapine, Clozapine and Haloperidol.
“The greater the number of medications you have, the increased risk of side effects and adverse effects. Those risks are not just additive, but they’re multiplicative,” Dr. Beach said.
“We had a feeling that he was being given excessive amounts of medication. But we had no way to know what was being given,” attorney Roppo said.
In December 2020, a judge appointed Kathleen to be her brother’s guardian, but Jimmy’s doctor continued to fight his release.
“He says ‘we’re not gonna let you ruin what we’ve done.’ And knowing that she has the guardianship,” Patty said.

“We located a place and wanted to transfer him there. It was way less restrictive than being in a hospital,” Roppo said.
An email from the local FACT team director describes the place, saying the home’s operator had “experience with caring for vulnerable adults with mental illness."
The email also said, “James has been calling our office daily requesting to move into a least restrictive environment.”
“He is held prisoner, essentially, in this hospital for one year’s time,” Kathleen said.
As the family awaited another court hearing to get Jimmy moved, he ended up back in the medical unit at Morton Plant with pneumonia and sepsis.
Patty Johnston says she remembers her final phone conversation with her brother.
“I heard I can’t breathe. He’s gasping for breath and he says whoever the woman was that answered the phone, another patient, he said tell my sister I can’t breathe. And I said I heard him. Hang up the phone. He needs your help. Call the nurse he needs help,” Patty said.
Jimmy died on March 23, 2021.
Doctor: Drug levels 20 to 50 times higher than upper limits
His death certificate listed natural causes including sepsis, pneumonia and other health conditions.
But a toxicology report that was part of a private autopsy paid for by his family raised serious concerns about the level of drugs in his body at the time of his death.
“I couldn’t believe the findings,” Roppo said.
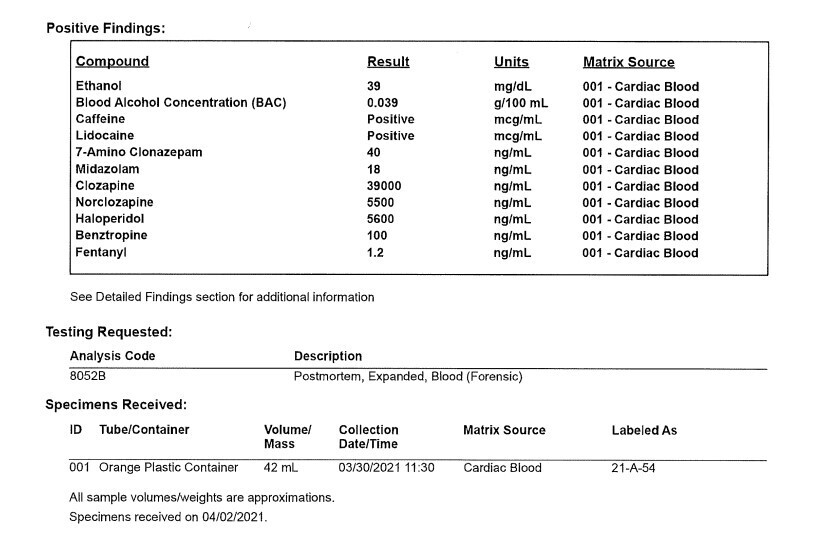
“The Clozapine level was around 20 times higher than the upper limit of that usual blood level range for Clozapine. And the Haloperidol level was around 50 times higher,” Dr. Beach said. “The levels were higher than some of those levels where fatalities have been reported.”
We contacted Baycare Health System, the parent company of Morton Plant Hospital, about the high levels.
A spokesperson said in an email, “While we cannot comment directly on any patient’s toxicology results, we do know that blood levels for some pharmaceuticals are significantly higher when drawn postmortem.”
We found published studies in which patients’ postmortem Clozapine levels were elevated by up to three times the levels found in blood tests while patients were alive.
But the autopsy report says the level of Clozapine found in Johnston’s blood was much higher than that, recorded at 39,000 ng/ml.
The report goes on to say, “in nine fatalities from Clozapine, postmortem blood concentrations were reported from 1,200-to-13,000."
Jimmy’s Clozapine level was three times higher than the highest level found in fatalities, all of which were determined from blood drawn after patients’ deaths.
Jimmy’s Haliperidol level was recorded at 5,600.
The toxicology report says “postmortem levels of Haloperidol in fatalities are typically greater than 1,000.”
“Those levels aren’t normal. There’s no way to pretend that they are,” Beach said.
$24,372.12 charge for medical records
The Johnstons say they haven’t been able to tell how often Jimmy’s blood levels were checked, since the hospital wants a fortune to access Jimmy’s medical records.
“We’ve been fighting for the records. We can’t even get Jimmy’s medical records,” Kathleen said.
The third-party vendor that provides records for the hospital is charging $24,372.12 for all of Jimmy’s medical records.
The family has received some information, including the hospital’s bill for Jimmy’s care, which totaled $1,194,583.08, about 90 percent of which was billed to Medicare.

Baycare said in the email that the bill “reflects a point in time for Mr. Johnston’s account before full review and reconciliation with payers’ policies.”
Kathleen says she’s reported the hospital to AHCA and the doctors to the medical board and police. She is still awaiting answers.
The family is unable to sue for wrongful death due to Florida Statute 786.21(8), nicknamed the “Florida Free Kill” law, which prevents families from recovering for pain and suffering and punitive damages related to medical negligence if the patient is unmarried and doesn’t have a child under 25 years old.
“I think it’s important to look at these cases, whether they’re fringe cases or not, and say the system didn’t work here,” Roppo said.
“If we don’t get justice for Jimmy, your family’s next,” Kathleen said. “Someone should be held accountable, but will anybody? I don’t know.”
A spokesperson says the hospital said during Jimmy’s time in the hospital the staff grew fond of him and called him “JJ”.
She said after his death, caregivers gathered in their department for a memorial service in his honor.
If you have a story you’d like the I-Team to investigate, email us at adam@abcactionnews.com





